Enrolled patients
Enrolment is currently available to residents in Auckland, Bay of Plenty and Canterbury. An enrolled patient is someone who has chosen Tend as their primary care provider.

Dr Sally McLaren leads a team delivering digital clinical services across Tend’s network and the model is reshaping how primary care workload is managed
When Dr Sally McLaren stepped into the role of GP clinical lead for Tend Health’s digital services in 2025, she was building on foundations she had already helped shape since joining the service in 2023. Two years on, her multidisciplinary team of 30+ GPs, nurse practitioners, prescribing pharmacists and nurses is quietly demonstrating what centralised clinical infrastructure can look like in primary care when it’s designed around safety and scale.
"We function as core clinical infrastructure across the Tend network," Dr McLaren explains. "Our digital service handles some of the work that strains in-clinic capacity: repeat prescriptions, overflow inboxes, clinical correspondence that has no allocated GP, and low acuity urgent presentations suitable for short video consults."
This isn't a call centre. It's clinical scaffolding that allows more than 150 GPs and as many other healthcare professionals across Tend's integrated clinics to focus on what requires their hands and eyes in the room.
What the numbers look like
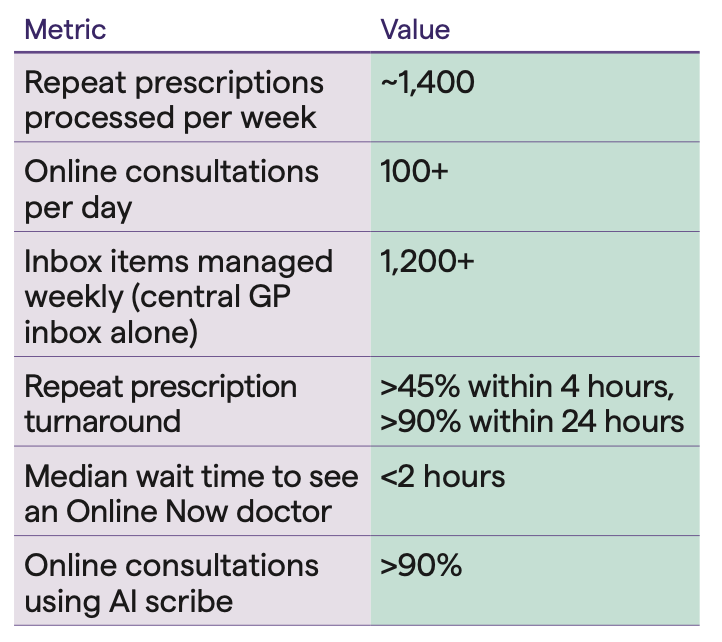
The team processes approximately 1,400 repeat prescription requests weekly, manages over 1,200 inbox items, and delivers more than 100 online consultations daily. This sits alongside a nurse-led medical certificate service for straightforward conditions and online mental health brief intervention consults.
"What we're really doing is freeing up in-clinic GPs to see their regular patients," Dr McLaren says. "And when you're centrally managing results and clinical correspondence for clinicians who are away, have left, or work part-time, you're preventing things from falling through the cracks whilst maintaining continuity of care.
"The scale of impact becomes concrete in specific cases. When Tend integrated the Ashburton practice, a single 0.8 FTE GP stretched across 4,500 enrolled patients,Dr McLaren's Central Clinical Team took over inbox management and repeat prescribing on day one, delivering a 56% reduction in administrative burden within the first month. Wait times dropped from 28 days to six. Patient satisfaction rose from below 70% to over 90%. That intervention was only possible because this infrastructure already existed.
Right skill, right work
The service operates on a skill-matching principle that Dr McLaren describes as one of the key design features. Pharmacist prescribers manage the majority of simple repeat prescriptions effectively. Nurses handle straight forward medical certificate requests and process certain inbox items such as clinic letters and hospital discharge summaries. GPs and nurse practitioners flex between consults, inboxes, and more complex clinical tasks as demand shifts. Each group works to carefully designed standard operating procedures tailored to their scope of practice.
"We have regular multidisciplinary meetings every three weeks with robust discussion where plans are made and implemented," Dr McLaren notes. "There's high team cohesion despite our geographic spread across New Zealand."
Clinical safety remains non-negotiable. The team conducts ongoing audits around prescribing quality, with pharmacists reviewing scripts and nurse inbox management regularly assessed.Repeat scripts typically turn around in under 24 hours, and results are actioned promptly without waiting for a named GP to return.
Capacity creation, not redistribution
The broader significance of Dr McLaren's team lies in what it represents for the workforce debate. Tend's own data shows that 88% of surveyed clinicians working in online channels report working additional hours specifically enabled by the digital model, with 44% maintaining workforce participation when they would otherwise have stopped practising in New Zealand entirely. Many of the clinicians in Dr McLaren's team fit this pattern — contributing clinical hours they could not or would not offer through traditional in-clinic practice.
The AI layer
In July 2024, Tend introduced its bespoke AI scribing tool across the network. Uptake in Dr McLaren's Online Now team exceeds 90%. The system creates high-quality open clinical notes made available to patients via the Tend app, reducing documentation burden and improving medical record quality. "The time saving matters, but for my team the real impact is on clinical safety," says Dr McLaren. "A multidisciplinary model depends on reliable documentation. When a prescribing pharmacist is processing a repeat script, the quality of the consultation notes is what makes that safe."
Looking ahead
"I feel really privileged to lead this clinical team," Dr McLaren reflects. "We have come such a long way since we started in 2023. We are already delivering complex clinical care safely at scale." The challenges facing general practice, capitation funding that lags behind costs, critical workforce shortages, rising chronic disease burden, won't be solved by individual clinicians working harder. They require the kind of clinical infrastructure Dr McLaren's team represents: multidisciplinary, technology-enabled, and designed to let every clinician work at the top of their scope. Two-thirds of Tend's consultations still occur face-to-face. But when centralised digital teams can safely manage the administrative and acute workload that overwhelms solo and small practices, they create breathing room for in-clinic GPs to do what only they can do, the physical examinations, the complex conversations, the longitudinal relationships that define general practice at its best. "Tend is good at looking forward to changes that can be made to improve systems," Dr McLaren says. "And I'm looking forward to being part of that."